Researchers from TU/e, Fontys Hogescholen and Rijnstate Ziekenhuis have developed a new bioluminescence-based sensor that can detect tiny amounts of viral or bacterial DNA/RNA in samples.
PCR testing – the highly sensitive gold standard for Covid-19 detection – requires expensive equipment, expert technicians, and dedicated laboratory facilities, all leading to test times of several hours or even a day. Researchers from Eindhoven University of Technology, Rijnstate Hospital, and Fontys University of Applied Sciences have developed a new test based on a ‘glow-in-the-dark’ approach that could be used to directly detect DNA/RNA of viruses and bacteria with the same sensitivity as a PCR test, and all in just 30 minutes.
“PCR testing is very accurate and was invaluable during the pandemic,” says Maarten Merkx, from the Institute for Complex Molecular Systems (ICMS), department of Biomedical Engineering, and head of the Merkx Lab at TU/e. “But it can take several hours, and often a day, to get the result of a PCR test.”
Part of the time delay with PCR testing, which checks for the presence of viral DNA or RNA in a patient sample, is the need for a thermal cycling process.
“Samples tested via PCR might contain miniscule amounts of viral DNA/RNA. To make this detectable, the sample is subjected to cycles of heating and cooling. This leads to the right conditions for DNA/RNA replication,” says Harm van der Veer, who is a PhD candidate in the Merkx Lab at TU/e. “But expensive equipment is needed, making it unsuitable for use by GPs or other local health facilities, let alone as a home test.”
Enter LUNAS
To address these drawbacks, van der Veer, Merkx and colleagues from TU/e, Rijnstate Hospital, and Fontys University of Applied Sciences have developed a new sensor that can be used at the GP, gives rapid results, and has similar sensitivity and specificity as the PCR test.
And just like the PCR test, their test has a catchy acronym. It’s known as LUNAS. Their work on the test has just been published in the journal ACS Central Science. Van der Veer: “LUNAS stands for luminescent nucleic acid sensor, which means that we have made a bioluminescent sensor to detect the nucleic acids (the molecules that make up DNA or RNA) found in viruses and bacteria.”
The Merkx Lab has considerable experience with bioluminescent sensors. “Many organisms such as fireflies use bioluminescence to produce light. In our sensors, we combine proteins that bind a certain biomolecule (such as an antibody or DNA or RNA) with so-called luciferase enzymes, which emit light upon detection of the target biomolecule in a sample,” says Merkx.
What’s more, bioluminescent sensors require no external excitation and the ‘glow-in-the-dark’ response can be detected with an ordinary digital camera that you’ll find in a smartphone.
A CRISPR helping hand
When developing LUNAS, the researchers had to solve two major problems: ‘How can the test replicate the thermal cycling amplification of DNA used in PCR testing?’ and ‘How can the sensor accurately bind to the resulting DNA in a rapid manner?’
“Our aim was a test with the sensitivity to detect a single piece of DNA in a microliter sample (a sample that is one millionth of a liter) that also happens to contains lots of other molecules. It’s like trying to find one specific, tiny fish in a sea of quadrillion (1015) liters of water filled with lots of other fish,” says van der Veer.
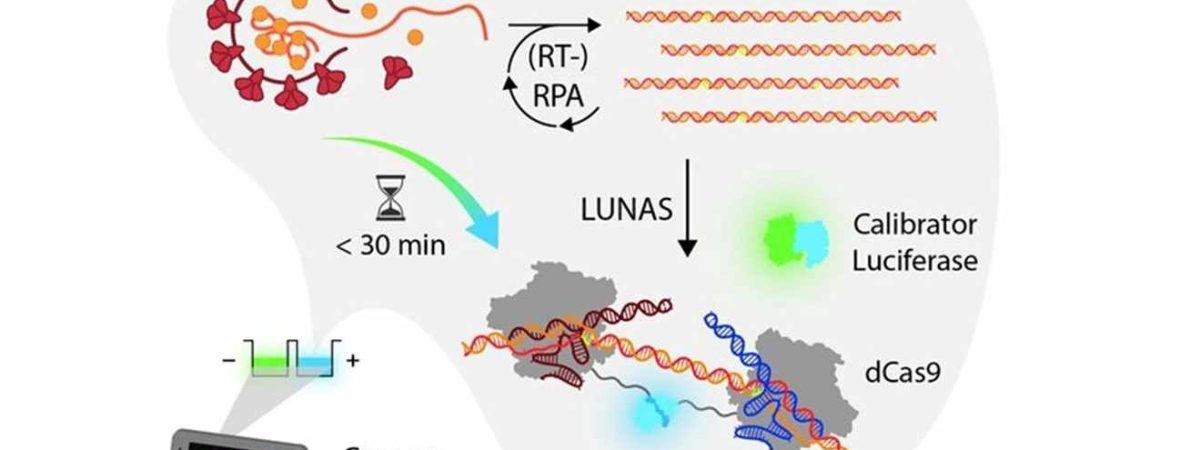
First, to quickly produce more viral DNA/RNA copies in a sample, the researchers used so-called recombinase polymerase amplification (RPA), which has been used in other point-of-care (close to the patient) tests in the past, as it works at low, constant temperature unlike PCR.
Second, to ensure specific detection of the DNA/RNA in the sample the researchers turned to CRISPR for help. “Most people associate CRISPR with DNA editing, but at the heart of CRISPR is a very accurate way of identifying and latching onto pieces of DNA”, says van der Veer.
So, the researchers bonded two CRISPR proteins to a split bioluminescent protein (See image). These proteins are designed to recognize and grab pieces of viral DNA copies. When they do so, the two pieces of the bioluminescent protein are joined together and produce blue light. Then, the researchers can detect the blue light using a digital camera.
If there’s no viral DNA/RNA in the sample, little or no blue light is emitted by the sensor. Instead, a reference bioluminescent protein just emits green light.
“However, when viral DNA/RNA is present, within about 10 – 30 minutes there is a marked increase in the blue-to-green light ratio. It’s like a molecular traffic light,” adds Merkx. To validate the accuracy of the LUNAS sensor to detect viral infections, the researchers tested Covid-19 patient samples provided by Rijnstate Hospital.
iGEM beginnings and future directions
LUNAS can be traced all the way back to the iGEM Eindhoven 2019 student project when van der Veer was part of the student team, which worked on making a test for the rapid detection of bacterial pathogens and help fight antimicrobial resistance.
From working on the project, van der Veer developed his interest in biosensors, which led to his masters research, and now PhD research, at the Merkx Lab. “The fruition of my time with iGEM is LUNAS,” says van der Veer.
LUNAS also looks set to be developed to detect other illnesses. “In a collaboration involving Fontys, companies, healthcare professionals, and led by TU/e PhD researcher Yosta de Stigter, we are developing LUNAS to test for sexually transmitted disease (STDs) and a portable microfluidic device to help with its use at point-of-care (near patient or beside) locations,” says Merkx.
Commercialization is also on the minds of van der Veer and Merkx, particularly for healthcare. However, there are key barriers to this adaption in healthcare.
“At the moment, we lack a simple and portable device for the test, which would make it easier for use at GPs or even at home,” notes van der Veer. “In addition, it would be great to have a commercial partner that could produce the tests at a large scale, while also accounting for all of the regulatory steps that need to be adhered to when making such a test.”