People treated with antibiotics are at heightened risk of having clostridium difficile infection as those drugs disturb the microbial balance of the gut.
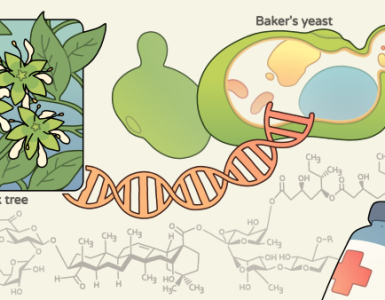
Clostridium difficile infection causes the most common and most dangerous hospital-born infections in the US and across the globe. People treated with antibiotics are at heightened risk because those drugs disturb the microbial balance of the gut, but observational studies have also identified a link between severe clostridium difficile infections and use of non-steroidal anti-inflammatory drugs (NSAIDs).
Understanding the severity of clostridium difficile infection
The researchers followed two groups of antibiotic-treated mice for one week after infection with clostridium difficile. One group had been treated with an NSAID called indomethacin prior to infection, and the other hadn’t. Only about 20% of the mice treated with the NSAID survived to the end of the observation period, compared to roughly 80% of the mice that hadn’t been exposed to the NSAID.
Even brief exposure to the NSAID prior to clostridium difficile inoculation increased the severity of infections and shortened survival. Further cellular and genetic analyses revealed that the NSAID exposure altered the gut microbiota and depleted the production of prostaglandins, hormone-like substances known to play an important role in gastrointestinal health.
Those observations align with previous studies reporting that NSAIDs can cause or exacerbate an inflammatory disease called colitis, also by inhibiting the body’s production of prostaglandins.
In the new study, the researchers conclude that NSAID-driven changes worsened clostridium difficile infections by impairing epithelial cells, the main defence system in the intestine against infectious taxa, and by disturbing the normal immune response. They studied at the impact of only one NSAID, indomethacin, but the researchers believe the findings might extend to other common NSAIDs, including ibuprofen and aspirin, since they all have roughly the same biological mechanism.
Study leader David Aronoff, a microbiologist and infectious diseases expert at Vanderbilt University, USA, explains: “Ultimately, these new results might guide how we treat people with C. diff, particularly with pain management.”
“Right now, it’s too early for our results to guide clinical care, but they should be a stimulus for future studies.”
Source: Health Europe