 HPV vaccination among those with autoimmune disease appeared low in new study
HPV vaccination among those with autoimmune disease appeared low in new study
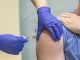
There are vaccines that protect against the human papillomavirus (HPV). These vaccines are often recommended for people with autoimmune diseases who are prone to infection. But it seems that many of these folks may not be getting the HPV vaccine.
HPV gets transmitted through sexual contact, and it can lead to genital warts and cervical cancer, as well as other types of cancers. Since 2006, the US Food and Drug Administration (FDA) has approved two vaccines for HPV in males and females between 9 and 26 years old.
Although research has shown the HPV vaccines to be effective and safe, a recent study reported that a low percentage of people were vaccinated for HPV, regardless of whether they had a history of autoimmune disease or not.
Candace H. Feldman, MD, from the Division of Rheumatology, Immunology and Allergy at Brigham and Women’s Hospital in Boston, MA, and colleagues recently examined whether people with autoimmune diseases were getting vaccinated for HPV.
Autoimmune diseases are linked with increased rates of infection with HPV.
The researchers gathered data on individuals between 9 and 26 years old with and without autoimmune disease using a US insurance database from 2005 to 2012. Data on 29,255 participants with autoimmune disease and 117,020 without autoimmune disease were examined.
Participants with autoimmune disease were found to have any of the following diseases: juvenile idiopathic arthritis, rheumatoid arthritis, systemic lupus erythematosus, psoriasis, psoriatic arthritis, inflammatory bowel disease, vasculitis, multiple sclerosis, dermatomyositis, scleroderma, ankylosing spondylitis, Goodpasture’s syndrome and sarcoidosis.
The study found that participants with autoimmune diseases had significantly more physician visits, abnormal Pap smears and sexually transmitted diseases than participants without autoimmune disease.
The FDA has approved two HPV vaccines (Cervarix and Gardasil), and it is recommended that these vaccines be administered in a series of three over a six-month period.
However, in both groups (with and without autoimmune disease), most of the participants didn’t receive the HPV vaccine. Specifically, the study reported that 8.5 percent of patients with autoimmune disease and 9.1 percent without autoimmune disease were vaccinated for HPV (at least one shot).
The percentage of people who completed the series of three was even lower — only 3 percent of participants in each group.
The study also inspected the number of participants who received the HPV vaccine by gender and geographical region of the US (Northeast, Midwest, West and South) for both groups.
More females received the vaccine (around 14 percent in each group) than males (1 percent in each group). And only about 5 percent of the females completed the three vaccine series, while only 0.1 percent of the males did.
No difference was found on vaccination intake between patients with and without autoimmune disease by geographic region, except for the Northeast. Among the participants living in the Northeast, those with autoimmune disease were more often vaccinated (16.3 percent) than those without autoimmune diseases (11.8 percent).
A total of 21 of the US states have regulations that promote or require HPV vaccination. This study reported that more people in the autoimmune disease group (7.1 percent) living in these states got vaccinated compared with those living outside the 21 states with HPV legislation.
The authors of this study wrote that vaccination can prevent HPV infections, and that vaccination is very important for those with higher risk for infections, such as people with compromised immune systems. They suggested that more information about HPV and health strategies are needed to promote HPV vaccination among preteens and teens.
This study has been presented on October 27 at the American College of Rheumatology Annual Meeting in San Diego.
Source: dailyRX