 Grappling with one of the world’s deadliest contagions for more than a decade without a breakthrough, the country’s leading infectious disease researchers have high hopes for a vaccine developed locally.
Grappling with one of the world’s deadliest contagions for more than a decade without a breakthrough, the country’s leading infectious disease researchers have high hopes for a vaccine developed locally.
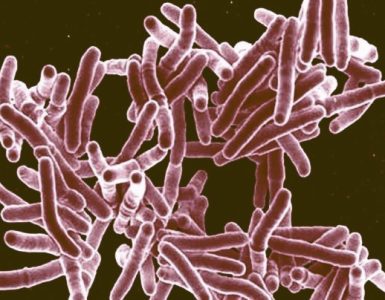
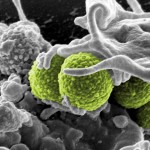
The NDV-3 vaccine aims to prevent deadly Methicillin-resistant Staphylococcus aureus (MRSA), which attaches itself to skin and embeds in bodily organs. The so-called superbug is responsible for more yearly deaths than HIV, tuberculosis and hepatitis combined.
MRSA is the leading cause of skin infections, which often migrate into the bloodstream. Open wounds are especially vulnerable, as are any kind of surgical implants such as a defibrillators, pacemakers or prostheses. Roughly one-third of infections result in death, and the bacteria are so adept at tricking human immune systems that infections spread easily in sterile hospital environments.
Dr. Michael R. Yeaman, an investigator at Los Angeles Biomedical Research Institute and chief of molecular medicine at County Harbor-UCLA Medical Center near Carson, introduced NDV-3 as a promising solution in a new report published last month in the scientific journal Proceedings of the National Academy of Sciences USA.
“The problem with Staph aureus is that many people have tried to create a vaccine, but it’s an organism that (naturally) lives in or on our bodies and it has a lot of ways to overcome or disguise itself against the immune system,” said Yeaman, chief author of the report. “The approach we’ve taken may represent an exciting new way to overcome historical challenges.”
Yeaman and other members of the development team for NDV-3 at NovaDigm Therapeutics believe a fungal protein called Als3 can mobilize the human immune system into a multipronged attack on the pathways that allow the bacteria to take hold. In lab tests on mice, results demonstrated that it prevents and reduces the skin and blood infections, according to their December report, “Mechanisms of NDV-3 vaccine efficacy in MRSA skin versus invasive infection.”
The vaccine, which is still undergoing clinical trials, is the first to target both MRSA and an associated fungus, Candida albicans, which causes infections that are also difficult to control. The two infections often occur at the same time and are growing increasingly adept at resisting anti-infective therapies.
But previous studies also have shown promise in early tests, only to fail later. NovaDigm’s next step is to test it on infected humans. The National Institutes of Health and the U.S. Department of Defense are paying for much of the research.
Staph hits particularly hard in the military, among collegiate and professional football teams and in prisons, long-term care facilities and other areas where groups of people are often in close contact.
“Staph is a tough bacteria, and it’s a tough business,” said Dr. Vance Fowler, an infectious disease specialist at Duke University Hospital who pioneered the failed Merck MRSA vaccine.
“The most chilling blow to the development of a Staph vaccine came with the project I was the lead author on in 2013. It sought to reduce MRSA in cardiac-surgery patients. Not only did it not work (in infected humans), but those with the vaccine were five times more likely to die. We don’t know why it happened.”
Uninfected humans tolerated the Merck vaccine in early trials, and it prevented infection in mice, making the final results a heartbreaking shock, Fowler said. The outcome had a “terrible effect” on a field that depends on massive financial investments from pharmaceutical companies, making the future of the NDV-3 vaccine and other promising scientific leads that much more intriguing.
Another once-promising vaccine by Nabi Biopharmaceuticals that attempted to prevent the infection from disguising itself to its host’s immune system also failed, despite high hopes, extensive research and huge financial investments.
Though a solution has been evasive, these attempts aren’t in vain, said Dr. Steven Projan, who has been studying MRSA for more than three decades and oversees research and development at MedImmune, a Maryland biotechnology company owned by AstraZeneca. He believes it’s imperative that a MRSA vaccine is found to prevent infection because antibiotics are losing efficacy as the microbial pathogens routinely outsmart and overwhelm them.
Projan is now working to neutralize toxins released by the bacteria. Pfizer has a promising vaccine in clinical trials now as well, along with several other pharmaceutical companies.
“Every time we take a novel vaccine or prevention approach into the clinic, we learn something more about the vaccine,” Projan said. “We’re understanding better what components we need to have from both an active and passive approach to prevent Staph. Figuring out approaches to make Staph vulnerable again is going to be key.
“It’s an amazing bug. But some of the failures have come really close to showing efficacy.”
Source: San Gabriel Valley Tribune