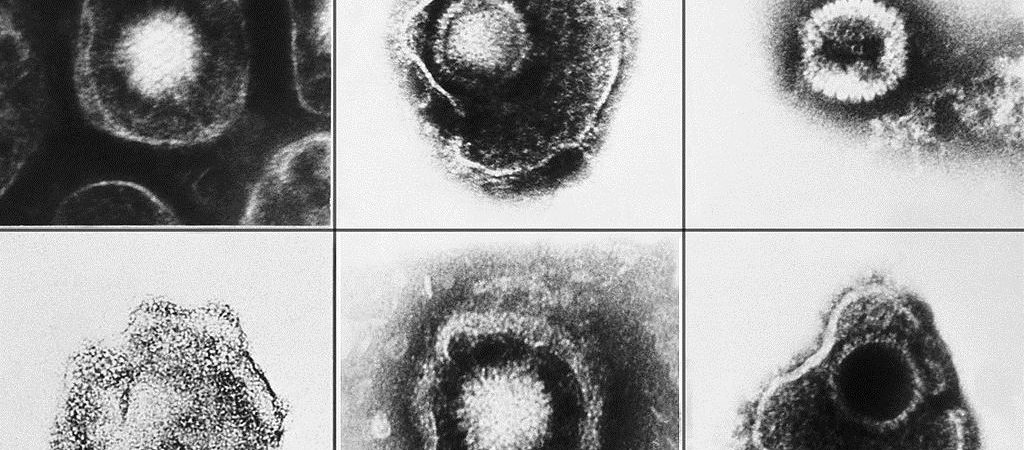
There’s a lot more “sex” going on between the oral and genital herpes viruses than scientists previously thought, according to a new study. The study, published April 23 in The Journal of Infectious Diseases, found that the two herpes simplex viruses — known as HSV-1 and HSV-2 — mix their genetic material together, or “recombine,” more often than thought. (HSV-1 classically causes oral infections and HSV-2 causes genital infections.) The researchers “found, basically, that there was considerably more recombination than had previously been appreciated,” between the two viruses, said study co-author Dr. Alex Greninger, an assistant professor of laboratory medicine at the University of Washington (UW) School of Medicine. What’s more, although scientists knew that the two viruses had mixed in the distant past, the new study shows that this mixing continues to this day. “Herpes viruses are still having sex,” Greninger told Live Science. But the mixing appears to be a “one-way”...
🔒 Premium Content - For Free
Unlock this content by becoming a Global Health Press subscriber. Join for exclusive articles, expert research, and valuable insights!