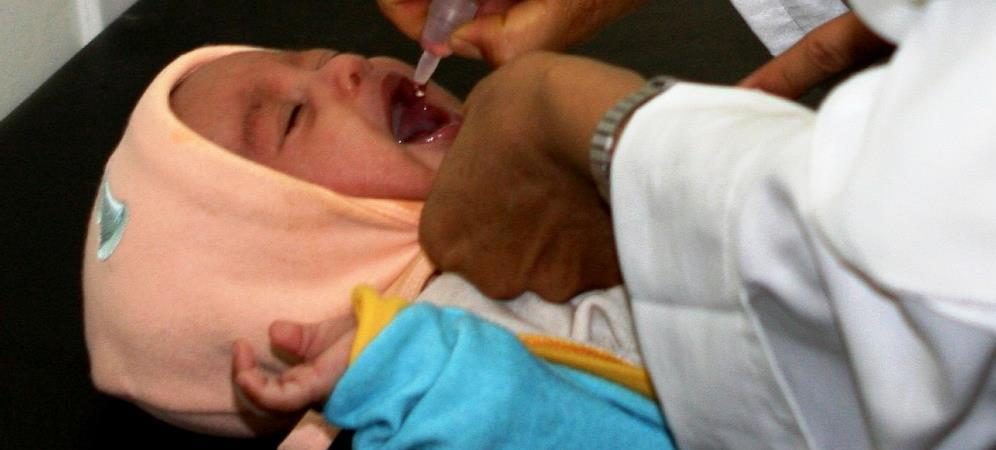
An orally administered vaccine can protect millions from hepatitis B: oral vaccines are both safer and less expensive than injections; researchers are continuously pursuing ways to produce an oral vaccine that is sufficiently effective. Millions of people are infected with hepatitis B every year. Hundreds of thousands die and small children are particularly at risk. Due to the high cost and the stable environmental conditions required for vaccine storage, many people in developing countries are not vaccinated against this dangerous virus. As such, researchers have been working to produce a drop or powdered form of oral vaccine. Oral vaccinations are cheaper and more easily administered than injections. However, developing a sufficiently effective oral hepatitis B vaccine has so far eluded researchers. A joint collaboration from physicists at the Niels Bohr Institute, a team of researchers from the University of São Paulo together with the Butantan Institute has introduced a technique to the...
🔒 Premium Content - For Free
Unlock this content by becoming a Global Health Press subscriber. Join for exclusive articles, expert research, and valuable insights!