Childhood vaccination for norovirus may reduce the community burden of norovirus outbreaks, according to a study published in Clinical Infectious Diseases.
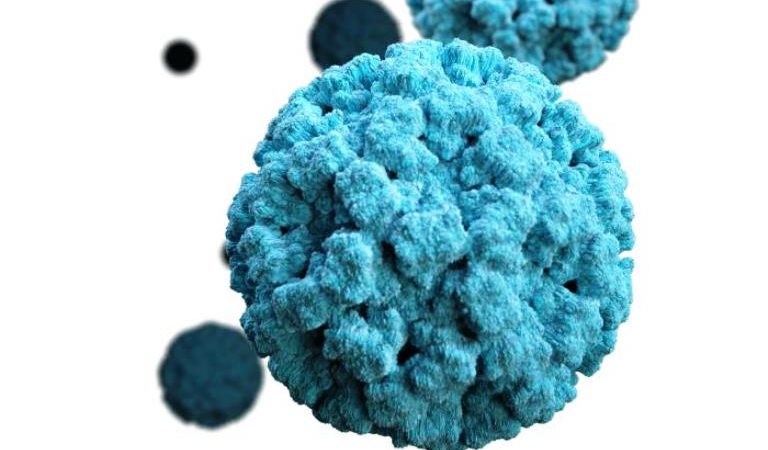
Norovirus is the leading cause of acute gastroenteritis in the United States, causing an estimated 20 million illnesses each year. Norovirus affects all age groups; however, severe illness is most likely to occur in vulnerable populations, including children. Norovirus is transmitted primarily via the fecal-oral route through the consumption of contaminated food and water or by person-person contact.
Currently, national norovirus surveillance is restricted primarily to outbreaks, rather than sporadic illness; however, multi-enteric pathogen testing has made sporadic norovirus surveillance more feasible. In Tennessee, acute gastroenteritis outbreaks are required to be reported and are identified and investigated by local health authorities.
Additionally, the New Vaccine Surveillance Network conducts active surveillance for medically attended acute gastroenteritis in children through a network of sentinel pediatric hospitals.
To improve preventative measures and assist in norovirus vaccine development, understanding norovirus transmission dynamics is vital; however, transmission dynamics between sporadic norovirus illness in the community and outbreaks are not well described. Therefore, the study investigators analyzed seasonal patterns and genotypic distribution between 2 demographically distinct surveillance populations (sporadic pediatric norovirus cases and reported norovirus outbreaks) in Tennessee to describe norovirus epidemiology.
Sporadic cases were ascertained via the New Vaccine Surveillance Network in a single county; reported norovirus outbreaks were ascertained from 7 Tennessee counties. The predictive value of sporadic cases on outbreaks was investigated using a 2-state discrete Markov model. In total, 3273 participants were enrolled and had stool specimens tested; 755 (23.1%) samples tested positive for norovirus and 81 (10.7%) of those samples had codetection of >1 other viral pathogen.
In total, 45 reported outbreaks occurred between 2012 and 2016. Approximately half of cases (42.2%) occurred in long-term care facilities. Among the pediatric sporadic outbreaks, 81.3% cases occurred in children aged <5 years, with an overall mean age of 2.9 years. The 45 reported outbreaks involved 1924 people, of which 28 (62.2%) cases were laboratory confirmed cases of norovirus. Age was reported for 740 cases of the outbreak, of which 45 (6.1%) cases were children aged < 5 years and 309 (41.8%) cases were people aged >75 years.
Results suggested that the temporal and genotypic characteristics of sporadic norovirus in the pediatric population were reflective of those among reported outbreaks in the greater region. Although norovirus outbreak can occur throughout the year, most cases occur between November and April; 75.0% of sporadic cases and 86.7% of reported outbreaks occurred during the winter season. Outbreak occurrence was often concurrent with peak sporadic norovirus activity. The most prevalent genogroup among both the sporadic and reported outbreak noroviruses was GII (90.1% and 83.3%, respectively), with the most dominant genotype being GII.4 (39.0% and 52.8%, respectively).
The predictive model suggested that the 3-day moving average of sporadic cases was positively associated with the probability of an outbreak occurring.
Cumulatively, the results demonstrated the temporal and genotypic interrelationships between pediatric sporadic norovirus vases and outbreaks in the same geographic region support the proposed effect of childhood vaccination on reducing the community burden of norovirus disease. Overall, the study authors concluded that, “Public health agencies may use this knowledge to expand surveillance and identify target populations for interventions, including future vaccines.”
Reference: Parikh MP, Vandekar S, Moore C, et al. Temporal and genotypic associations of sporadic norovirus gastroenteritis and reported norovirus outbreaks in middle Tennessee, 2012-2016 [published online November 13, 2019]. Clin Infec Dis. doi:10.1093/cid/ciz1106/5624073
Source: Infectious Disease Advisor