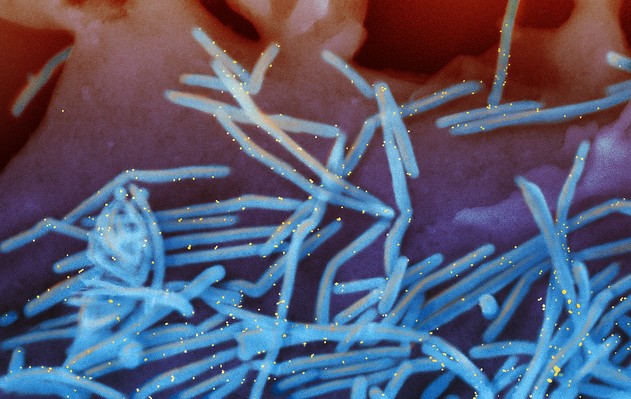
Respiratory syncytial virus (RSV) is common cause of infections such as pneumonia. Most cases and deaths in young children occur in lower-income countries. Passive immunisation campaign urged for babies under six months. As COVID-19 and monkeypox hog the limelight, new research sheds light on the devastating potential of another viral disease—the respiratory syncytial virus (RSV)—that kills more than 100,000 children a year worldwide. RSV is the most common cause of acute lower respiratory tract infections in infants and young children around the globe, but the burden of disease is disproportionately high in developing countries, according to the Respiratory Syncytial Virus Consortium in Europe. Lower respiratory infections affect the airways below the larynx or voice box, including the windpipe, or trachea, and tiny air sacs in the lungs. They include acute bronchitis, bronchiolitis and pneumonia. Figures published in The Lancet reveal that more than 95 per cent of incidents of acute lower respiratory infection associated...
🔒 Premium Content - For Free
Unlock this content by becoming a Global Health Press subscriber. Join for exclusive articles, expert research, and valuable insights!